How to manage hormones and appetite.
- Gabriella Rachel Appanraj

- May 18, 2022
- 6 min read
Updated: Jun 20, 2023
I always have my appetite with me at all times, so just passing by some food that I love was never an option. But I soon learned to put them under subjection when I learned that some hormonal diseases are caused by excessive eating and carelessness.

I have been fascinated about and by hormones ever since I got diagnosed and later cured of PCOD by having enough sleep and healthy food at the right time. Since then I began to understand the role of hormones in any unhealthy condition that I became aware of.
Let me start off by introducing to you my friends called leptin and ghrelin who helped me massively to overcome this condition.
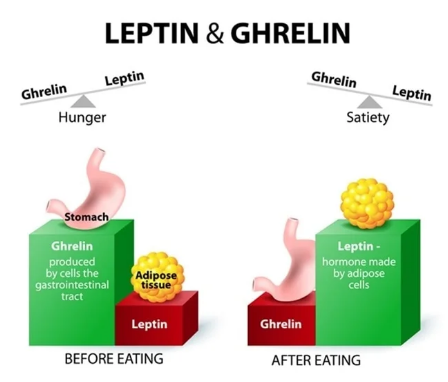
Leptin is a satiety hormone that decreases your appetite. It signals the brain that you have had enough food at the time. This should lead you to stop eating. Whereas ghrelin is a hunger hormone that increases your appetite rush. It instructs you about your lack of food and signals that you eat soon.
I befriended both of them, unlike some people who would love leptin more than ghrelin because of its role in decreasing the appetite. There has to be a balance maintained between these two “appetite hormones” in order to maintain a healthy body weight.
Roles of the appetite hormones
Leptin (satiety hormone) made by fat cells is present in fewer quantities in people who are thin and in high quantities in people who are fat. It might make you wonder- “If leptin is produced more in obese people, why do they have more appetite than people who are not obese?” The reason behind this is that obese people have built up resistance to the appetite-suppressing effects of leptin. In spite of having a higher level of leptin, obese people become insensitive to its function (appetite suppression).
Our next friend, ghrelin (hunger hormone) is released in the stomach and sends the hunger signal to the brain asking for food. Normally, ghrelin levels are higher before eating and lower after eating (for about three hours after a meal). Even though people with obesity have low ghrelin levels they are more sensitive to its effects (appetite induction).
Communication between the brain and appetite hormones

Leptin being an appetite-suppressing hormone sends information to the regulatory centre of the brain (hypothalamus) after being satiated during a meal. The hypothalamus of the brain then signals the body, saying that it’s full. The body starts to expend energy by increasing the metabolic rate and body temperature.
Ghrelin does exactly the opposite of what leptin does. Ghrelin sends information to the brain causing it to tell the body to seek out food. The body takes in food energy and uses it for the work required, and the rest (if there is more) is stored first as glycogen in muscles and the liver. And if the food is more again, they are further converted and stored as fat especially if they are of carbohydrate sources. Interestingly proteins don't get stored.
The levels of ghrelin ordinarily would increase before the meal which is part of what we interpret as hunger, and it decreases after the meal since you have now eaten.

Leptin resistance leads to obesity.
Given the way leptin is supposed to work, many people with obesity should limit their food intake. However, it is not about the leptin level but about the leptin signalling and the body’s sensitivity to it. Obese people become insensitive to leptin. While copious leptin may be present, the brain does not see it.
In a literal sense, the doors of the brain (leptin receptors) can’t hear the knocking on the door to allow the leptin inside. This renders the hormone useless even if it is present. The surplus leptin in circulation causes decreased glucose uptake by the muscle and increases glycogenolysis, and gluconeogenesis resulting in hyperglycemia which makes a patient vulnerable to type II diabetes.
Leptin levels are elevated in the body during sleep (including daytime sleep) as long as you took a meal before sleeping which makes us narrow down the reason why people put on weight if they sleep or are mostly sedentary after a meal.

What causes leptin resistance?
Both genetic and lifestyle factors contribute to low leptin signalling but the contribution of each factor varies widely from person to person.
The major lifestyle factor that causes leptin resistance is a high–fat, energy-rich diet. In an early stage of high-fat energy-induced obesity, increased amounts of saturated fatty acids cross the blood-brain barrier, causing the target cells in the brain to not respond to leptin signalling the brain to order the body to stop consuming food by suppressing appetite.
Changes in the leptin gene can also be the cause of less leptin but the chances of mutation in the leptin gene are very less.
Oversecretion of ghrelin leads to obesity.
Overweight people have more levels of ghrelin. Although the exact mechanism is not fully studied yet. So the same amount of ghrelin makes them hungrier compared to their normal colleagues. Therefore, ghrelin does not cause obesity instead the hypersensitivity of the brain cells to ghrelin does cause obesity.

In overweight people, ghrelin levels reduce much more slowly than in normal people after eating food. That keeps them hungry longer, making them overeat. Ghrelin also regulates blood glucose levels by reversing the effects of leptin resistance by reducing insulin secretion and regulating the synthesis and breakdown of glucose and glycogen.
It was also noted that when obese people lose weight, ghrelin levels show an increase as if to compensate for the weight loss.
Ways to regulate appetite hormones.
Obesity, genetic predispositions or health conditions, diet, sleep and lifestyle can throw our hunger and satiety out of whack, as well as compromise how efficiently our hunger hormones function.
The good news is, that there are many modifications you can make to get your leptin and ghrelin levels and effectiveness back to where you’d like them to be--under control.
1. Choice of food:
Eating fatty foods doesn’t lower ghrelin levels as quickly as proteins and carbohydrates do. Instead, it puts you at risk of being loaded with increased fat content in your body. So if you eat any food with high-fat content, your hunger may not reduce as quickly and you are likely to continue eating for a longer period. Having protein-rich and complex carbohydrates can surely help instead as they provide healthy timely energy. Avoiding highly processed foods might also help you with gut health and avoid inflammation. Also, make sure you eat varieties.

2. Food portioning:
As much as the phenomenon of hunger and satiety are completely involuntary, the portioning of the food you eat must always be in check especially when you are an inactive person. You do not want to overeat very frequently, which will cause your body to be insensitive to leptin signals over time. This, in turn, can further lead to becoming overweight and eventually susceptible to other lifestyle diseases like obesity, hypertension, fatty liver disease, heart diseases, dementia, stroke, and even cancer.
3. Nutrient content of the diet:
Carbohydrates and proteins lower your ghrelin levels quickly after eating. But since carbs are much maligned in obesity, it is a good idea to have high protein content in your meals.

Aim for 20% of calories from protein in a meal. Beans and vegetables such as cauliflower and green beans are good sources of insoluble fibre that decrease ghrelin levels post-consumption. Eating protein-rich food was proven to make the body sensitive to leptin.
4. Adequate Sleep:
Sleep properly for 7 to 9 hours. Lack of adequate sleep has been associated with higher levels of ghrelin and leptin insensitivity leading to hunger, weight gain and hyperglycemia.
5. Exercise:
Do some resistance exercises to increase your muscle mass. Higher muscle mass is associated with lower levels of ghrelin.
6. Avoid Fasting:
Finally, avoid extreme diets that restrict calories to less than 800 calories a day. You might lose weight rapidly but you will gain it back again because your ghrelin levels will be skyrocketing, making you very hungry. A few intermittent fastings are not bad at all, but fasting, in this case, will mean extreme starvation of food for a long period.

7. Lowering triglycerides:
Having high triglycerides can prevent the transport of leptin from your blood to your brain. The best way to lower triglycerides is to replace saturated fats such as whole-fat dairy products, red meat and ice cream with healthy fats such as olive oil, nuts, seeds (flax seeds) and soymilk.
Conclusion
I strongly believe that every one of us should treat our bodies with love and care. To cherish the body is to put the right fuel (healthy food) into it in order for it to run efficiently for a long period of time. I hope the article helped you to understand the internetworking between leptin, ghrelin and insulin in regulating appetite.
Let us not just be the readers of the article but be doers of it. Decide today to put at least three of the six remedies that are mentioned above into action for a period of 21 days. I am pretty sure your appetite friends will help you gain overall health.




Comments